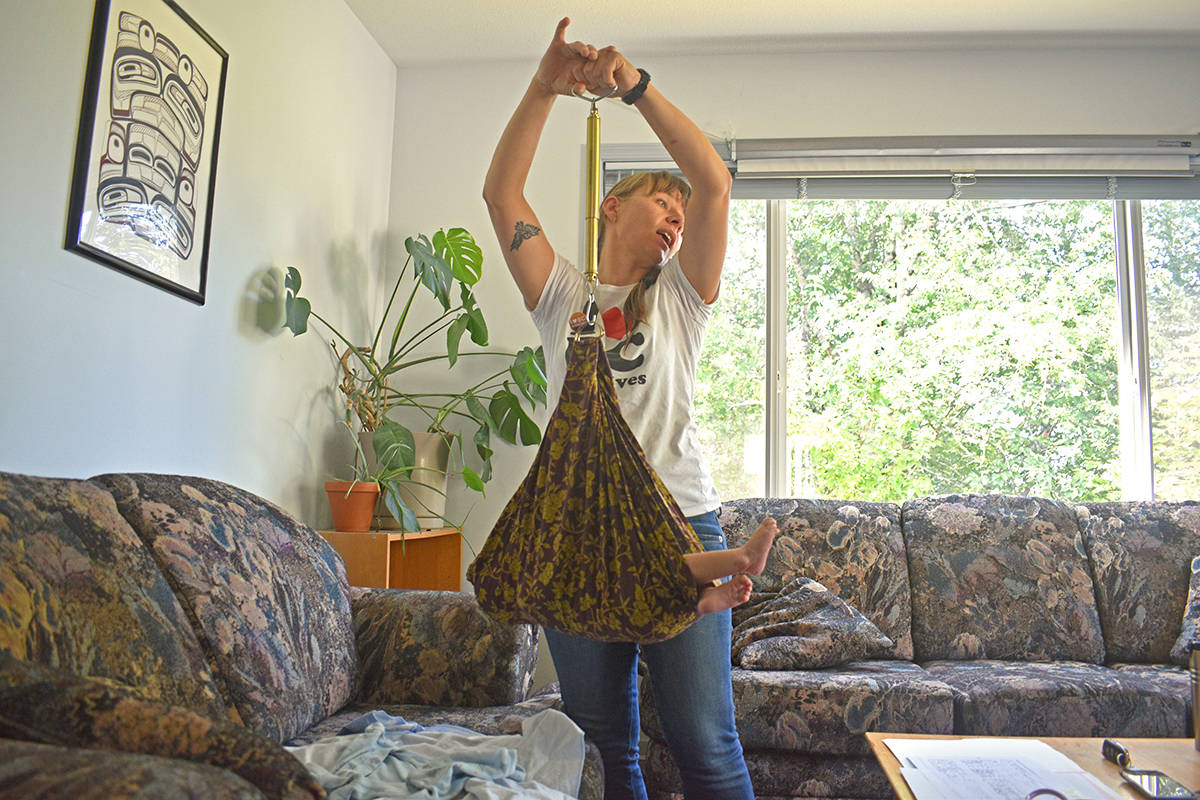A registered midwife looking to gain hospital privileges in Terrace was told Northern Health would not endorse her credentials to establish a clinical practice here.
Katherine Puchala has only been able to provide prenatal and postpartum care for mothers in northwest B.C. for the last year, and is the only midwife with a practice within reasonable distance to Terrace, Kitimat and Prince Rupert.
“I expect that by the end of the year, I will have had more than 40 people in my care,” Puchala says.
For the last year, Puchala has been going through the process of obtaining hospital privileges at Mills Memorial Hospital. This is important, considering an average of 70 per cent of births attended by midwives occur in hospitals, according to the BC Midwives Association. Without privileges, Puchala can’t deliver babies at home or at Mills.
Instead, she can provide care within the first and second trimester before consulting with the prenatal clinic for the third trimester. When it comes time to give birth, the mother’s care is transferred to a doctor at Mills and then transferred back to Puchala once they’re discharged from hospital.
READ MORE: Choosing what’s best for baby
In late January, Puchala says a senior Northern Health medical health official told her she would receive medical privileges within three days, but it wasn’t until April that she was called back for the final verdict.
“I was told there was an issue that came to light in my final reference check, and showed that I am not going to be a good fit here,” Puchala says. Though she says she doesn’t know the specific reason why, and Northern Health did not tell her, citing confidentiality.
“I have since talked to all of my references…none of them had any clinical concerns about myself,” she says. “I was incredibly confused and disappointed.”
Currently, midwives hold privileges in a number of communities in the region, including Prince George, Smithers, Dawson Creek, Hazelton, Village of Queen Charlotte and Masset. But there is a gap in service in the Skeena coast area of northern B.C., leaving expectant mothers who want the option of a midwife no choice but to travel hours outside of their community to get it.
Prince Rupert Advocates for Midwifery wrote a letter to the Minister of Health in July to express their disappointment in Northern Health’s decision and to request an investigation into the matter.
“In a provincially regulated health care system it is a woman’s right to ask for and receive the highest quality maternity care, and we believe that midwives provide this in consultation with doctors and obstetricians when necessitated,” the letter reads.
“Here is a situation where a registered midwife is eager to work in a small town in Northern BC with a demand for midwifery care and a shortage of doctors who provide maternity care, and yet her hospital privileges were not approved.”
READ MORE: Advocacy grows for midwifery services in Prince Rupert
Northern Health says they cannot comment on Puchala’s specific application because of privacy policy, but they recognize it is important for mothers in northwest B.C. to have access to midwifery care.
“We have midwives that hold privileges in communities across the region…we very much appreciate that they have an important role to play in making sure families have a choice in, and access to, prenatal, intrapartum and postpartum care,” says Eryn Collins, Northern Health spokesperson.
The health authority is currently conducting a midwifery review involving a variety of stakeholders to look at demographics, demand, the need for midwives to practice collaboratively with care providers and practitioners, and recruitment. A final report is expected late this year.
Collins also says there is another midwife in Terrace going through the privileging application process with the hopes of starting a practice.
Earlier this week, Terrace mother Megan Brooks met Puchala at the Terrace Women’s Resource Centre for a postpartum appointment following the birth of her fourth child two weeks ago. These appointments are usually done at the family’s home, but due to the presence of a Terrace Standard reporter the mother chose the resource centre for privacy reasons.
Puchala took newborn Walter into her arms and gently placed him on the couch. She measured his vitals, measurements, reflexes and weight while Brooks watched her daughter play nearby.
Puchala says she talks to her clients about mental health, breastfeeding, sleeping schedules, pain management in the early postpartum period, and other aspects of pregnancy with frequent follow-ups. After delivery midwives usually follow up with new mothers within 24 hours. The cost of a midwife is also covered through B.C.’s Medical Services Plan.
READ MORE: Bring midwifery to Terrace
As a mother of four, Brooks says she prefers the midwifery model of care over hospital maternity care.
“I wouldn’t see anyone professionally until the baby was six weeks old,” Brooks says. “When I had more than one [child], I’d have to drag the others along, bringing two to three children with me into the doctor’s office.”
The continuum of care throughout her pregnancy was what made midwifery attractive, she says. Even though she had to switch over care to the hospital once it came time to give birth, Puchala was there in the room with her to act as a doula, or a birth coach.
“I just held on to the fact that I knew my husband would be there and Katherine would be there, so even if I didn’t know anyone else in the room, I knew the two people I picked to be there would be there,” Brooks says.
Despite the outcome of her application, Puchala says having physicians work collaboratively with midwives can help bridge maternity care gaps. Recruiting and retaining doctors in this part of the province can be challenging, and new physicians aren’t required to also provide maternity care. Midwifery can be a collaborative solution to ease the onus on family physicians, she says.
“Midwives are specialists, pregnancy and birth are what we specialize in. We know that our schedules are going to be erratic. We make provisions to try and have some balance in our own lives, but we know that we care for pregnant women only.”
brittany@terracestandard.com
Like us on Facebook and follow us on Twitter