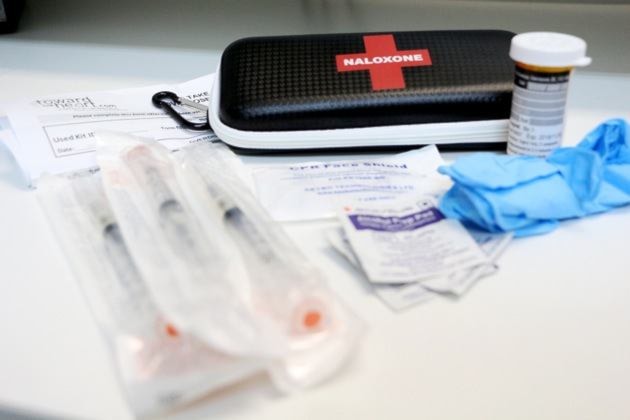
A drug that reverses the effect of fentanyl, heroin, methadone and other opioid drug overdoses is now available for users at the Northern Health public health clinic.
Naloxone, also known as Narcan, is an antagonist to opioids. Once injected, naloxone reverses the effect of an opioid drug by binding to the same site in the brain where the opioids bind and pushes them out. The drug reversal works for 15 minutes and wears off in 30 minutes, giving emergency responders enough time to reach the person in crisis.
“It can be a feeling of absolute terror and helplessness when you’re watching someone overdose and waiting for the ambulance to come and there’s nothing you can do in the meantime to save their life,” said the Northwest Medical Health Officer, Dr. Raina Fumerton.
The take home naloxone program has been available in other areas in the province, including Vancouver, Victoria and Kelowna since 2012, and on June 24 Northern Health trained team leaders at its public health clinic in Prince Rupert.
“As bad as it is, the overdose crisis would be a lot worse right now if we didn’t have take-home naloxone,” Dr. Fumerton said.
The crisis she refers to is the public health emergency declared by the provincial health officer in April, and two weeks ago the B.C. Coroners Service reported 371 people died from illicit drug overdoses in the first six months of the year, a 74 per cent increase from last year.
Overdose deaths in Prince Rupert
There have been five illicit drug overdose deaths in Prince Rupert, and the B.C. Coroners Service recently updated its report to include that fentanyl was a factor in one of those deaths.
Mysti Bateham is one of the two interprofessional team leaders here at the Prince Rupert Health Unit who is launching the take-home naloxone program. She explained that anyone who comes into the harm reduction centre at the health unit can receive efficient training from the nurses. She can also schedule in a group who wants to be trained.
The Salvation Army is one of the groups in town who has expressed interest in receiving training. Anyone can be trained in administering naloxone and how to help someone who is overdosing, but the kit is only available for users.
In March, naloxone became available in B.C. without a prescription, but the take-home naloxone program offered by the BC Centre for Disease Control (BCCDC) still requires a prescription from a physician. It’s not meant to be a barrier, rather the reasoning is to monitor the product offered to users free-of-charge at approved sites.
“It’s highly tracked. A person is only allowed five kits per year. That being said we’ll give you more,” Bateham said.
She’s never had to use the kit herself but she explained that it’s a simple process. Each kit has a black case, a CPR face shield, alcohol pads, gloves, a user form, three syringes with needles that retract once inserted into the muscle — and the naloxone.
Dr. Fumerton and Bateham also dispelled some of the myths or misperceptions on naloxone. “It’s very safe. It’s not a medicine that can be abused. It’s only action is to reverse the effects of opioids,” Dr. Fumerton said.
Former addict remembers his experience with naloxone
A former drug addict in Prince Rupert who has been clean for one year after 40 years of using, since starting the opioid substitution program, offered by Northern Health, said he has overdosed more than 20 times in his life.
John Davis, whose name has been changed, and whose story was featured in an article earlier this month, explained his experience with naloxone.
“Oh man, it was brutal. I was just shaking like a fish out of water flipping around when they shot me up with it. You get mad at the doctors and nurses because they wrecked your high,” he said.
Firefighters get trained
In the first six months of this year, the BC Emergency Health Services reported that ambulance services used naloxone 27 times for “suspected overdoses or poisonings” and there were 59 for all of last year in Prince Rupert.
Starting this year, firefighters also started carrying the kits to give naloxone to people suffering from an opioid overdose.
Prince Rupert Fire Chief Dave Mckenzie said it’s a program he wanted get going for the community. “For our size of community there has been a number of fentanyl cases and overdoses,” he said.
They are in the process of getting the training kits delivered to the fire department to train and certify their first responders.
“All this is just another tool in the toolbox,” he said.
The senior provincial executive director of medical programs and clinical initiatives at BC Emergency Health Services, Barb Fitzsimmons, said they have already trained 45 fire departments in the province including the fire chief and deputy fire chief in Prince Rupert who received training on June 18.
“We’re training the fire department trainers and they’re training staff on how to administer. They explain what happens in an overdose, how the body responds, how the naloxone counteracts the drug that they’ve overdosed on, which drugs it works on, because it can’t be used with every drug,” Fitzsimmons said.
There is also 24-hour physician support for firefighters who want to confirm whether or not it’s appropriate to administer naloxone when they encounter a person who has overdosed.
Police officers will not carry the kits, Fitzsimmons said. The BC Emergency Health Services doesn’t want people concerned that they’ll get arrested and would rather they call to save a person who has overdosed.