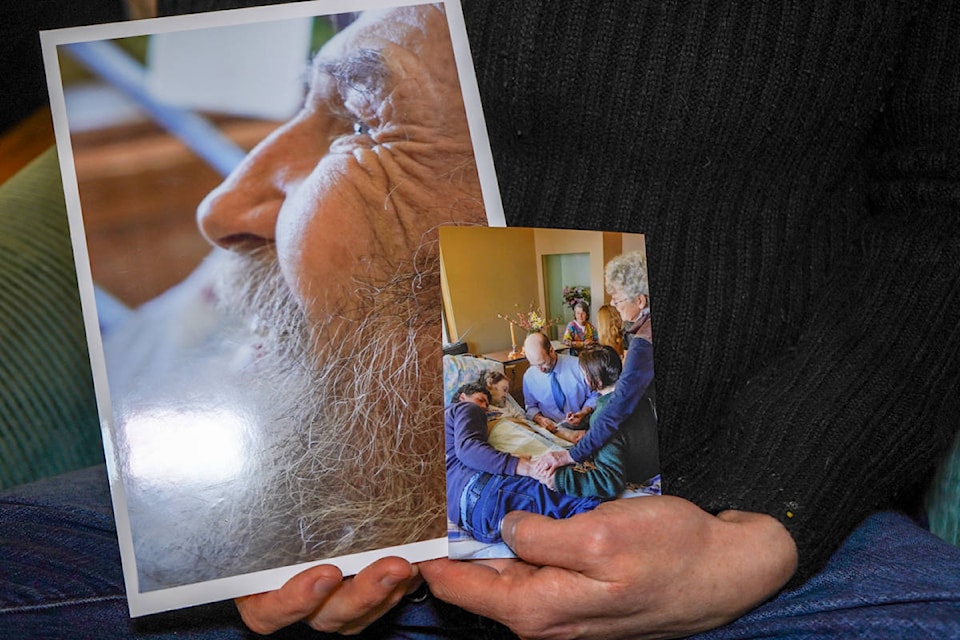
On Nov. 28, Chelsea Keays shared her family’s story on “medical assistance in dying and how to bury your own dead” at the Prince Rupert library.
This past spring, she travelled to Lund, a remote seaside town on the northernmost point of the Sunshine Coast. This was where her father lived, and where he chose to die.
His kidneys were failing him, and his doctor told him that he would die some time within the next year.
“Dad went home and went on living and dying both at the same time. After several months he was at a point where he was bedridden,” Chelsea said from her home in Prince Rupert.
Her brother mostly looked after their father, John. When John got to the point where he couldn’t control his bowels or clean himself, he said he was ready to die.
Medical assistance in dying became legal in June 2016. Since then, 62 people within the Northern Health region have chosen to end their life with medical assistance. The criteria for medical assistance in dying (MAiD) is when there is “grievous and irremediable” medical conditions.
When Chelsea presented her family story at the Prince Rupert library, months after her father’s death, one attendee said that the criteria seemed like it was broadly interpreted in her father’s case.
“In my dad’s case, the grievous suffering was emotional and psychological and it was connected to that loss of dignity,” she said.
For residents within the Northern Health authority, physicians and patients are supported through MAiD Care Coordination. Patients are connected with a participating physician, who may or may not be in Prince Rupert. But the service would be provided locally.
John was connected with a participating physician through the Vancouver Coastal Health authority. There was one doctor in Powell River, and more who were willing to do the assessment, but not the death day.
In the end, it was a physician from Comox who would travel by ferry and then car, to provide the service at her father’s home in Lund.
But first, John had to make an official patient request that had to be signed by two witnesses who aren’t family and aren’t health care providers. A barrier to some, Chelsea said, but not for her family.
Her father went through two assessments, with a 10-day period of reflection in between. The second assessment was by Skype on a phone, it was the first time her father had ever used such technology.
One of the things her father said to the doctor was “thank you so much for deciding to make this part of your practice and to make it available to people like me.”
Between Jan. 2016 and Oct. 31, 2018, there have been 1,644 medically assisted deaths across the province. The Island Health Authority has the highest number with 692 medically assisted deaths, and then Vancouver Coastal Health with 357 medically assisted deaths.
“Throughout my life I knew that my dad would sooner take his life than go to a hospital or go into care when he was at a point of real illness, and I thought of what that would be like,” Chelsea said, adding how someone would have to find his body.
But after assisted dying was made legal she didn’t have to imagine anymore, and she said the choice her father made was a positive experience.
RELATED: B.C. woman: Being in control of death a ‘civil right’
Death day
Once the doctor arrived in Lund, he assessed John one more time and asked him to give written consent to proceed.
The nurse put an IV in each arm, one as a backup.
The family gathered around his bed, and played “Calling all angels” by KD Lang and Jane Siberry, a song he wanted to listen to while he was dying.
“The nurse was right there and handed medicine to the doctor. At the last minute, he said, ‘John, I’m going to put a saline solution in to make sure this port is open. And dad said, ‘I’m not supposed to be having too much salt.’
“It was this moment of levity in an otherwise very somber time and it was so funny, we all laughed,” Chelsea said.
Before he received the second drug that put him to sleep, they shared their final words.
“He looked at all of us and said ‘I love you, goodbye’, we looked at him and said ‘We love you, goodbye’ and then those drugs started to take the effect.”
His head fell to the side and he snored.
“He looked like a baby falling asleep in a way, just so fast and so complete,” his daughter said.
He was given a third drug, which puts a person in a coma-like state where most people die, but just in case a fourth drug was administered that stopped the heart completely.
The whole procedure took less than 10 minutes.
“It was painless for my dad, as far as I could see, and it was completely peaceful. It was really beautiful.
“We all had our hand on some part of his body and he was completely alert and conscious and aware. For me that was one of the most amazing parts,” Chelsea said.
The family then took care of the burial, preparing his body and digging his grave, honouring his request.
The Supreme Court of Canada’s 2015 ruling to legalize medically assisted death was not without controversy due to some religious, ethical and professional sentiments. The physician who supported John’s decision encouraged the family to share their story openly with others who may have questions about the experience.
Which is exactly what Chelsea has been doing.
RELATED: A personal look at assisted dying